Nonprofits
SOMOS Community Care moves forward after helping NYC’s most vulnerable residents during COVID-19
The nonprofit bills itself as the largest, physician-led network in the five boroughs.
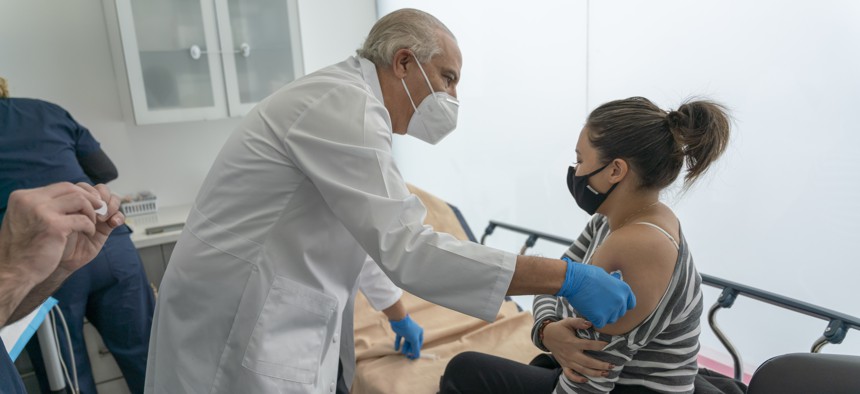
SOMOS Community Care Founder Dr. Ramon Tallaj pictured with a patient. Photo courtesy of SOMOS Community Community Care
SOMOS Community Care, the largest, nonprofit physician-led network in New York City, serves nearly one million Medicaid and Medicare beneficiaries from the city’s most marginalized communities. Offering culturally competent health care to primarily immigrant communities, such as Hispanic, African American and Asian Americans and Pacific Islanders communities, as one of the 25 Performing Provider Systems in the city’s Delivery System Reform Incentive Payment program, SOMOS has helped deliver affordable healthcare to individuals in need through state and city-subsidized independent health plans.
As COVID-19 hit New York, SOMOS remained on the frontlines with doctors providing testing at 70 trilingual sites and administering over 1.5 million vaccines across all five boroughs, while providing food to close to 2 million patients. Dr. Ramon Tallaj, the founder of SOMOS who also led the organization through the pandemic, received an Emmy nomination for a documentary chronicling SOMOS’ efforts during the early days of COVID-19. Additionally, he serves as co-chair on Mayor Eric Adams COVID-19 Recovery Roundtable and Health Equity Task Force, where he advocates for value-based care with an emphasis on holistic approaches to health and wellness.
Recognizing July as National Minority Mental Health Awareness, SOMOS employed a pro-active, integrative approach to mental and behavioral health services to identify early signs of depression and anxiety through free PHQ-9 and GAD-7 mental wellness screenings. SOMOS physicians also provided early interventions and referrals.
NYN Media caught up with Tallaj about SOMOS’ work and how the organization weathered COVID-19, as well as how it's now moving forward in its mission to provide accessible healthcare for marginalized communities.
This interview has been edited for length and clarity.
The COVID-19 pandemic was an especially difficult time for New Yorkers, particularly communities of color that were disproportionately affected. How did SOMOS respond to these challenges and how did this experience shape the future of your organization?
Right away, we opened testing centers in Queens with opposition from the authorities. People were afraid of what was going on but we told them it's all about testing. We spent almost $34 million of our money and were able to do more than 2 million in testing. With this healthcare crisis, people had no jobs, no insurance, there was no food and all their savings were gone by the first few weeks. In response, we gave more than 2 million meals to the city of New York. Our values were to remain open because we knew what the needs were. We lost 12 doctors since the beginning of the pandemic due to COVID. As for the future of SOMOS, we tell authorities that we should be an equity network for our neighborhoods. Our healthcare system in the United States is based on disease, where the building cohorts are the most important and the sicker you are the more money healthcare makes from it. We keep saying no. We need to keep people healthy so they avoid going to the buildings. I believe that we are getting somewhere because the mayor [Eric Adams] has made me in charge of the equity Task Force. We're working close with the governor to open peoples’ minds which is important for those who are sick and for certain changes that are needed. But we should do more wellness and prioritize happiness in the community, not complicated evaluative care.
You mentioned that you were appointed co-chairman of the New York City's recovery roundtable and Health Equity Task Force. What are some of the initiatives that you’ve been working on?
From the beginning, we talked about [popularizing] pure foods diets, and now we're working with trash [disposal]. Everybody, everywhere, knows that our buildings, our service stations, any apartment building in New York is filled with cockroaches and rats. And we don’t do anything about it. We need to start with the garbage. That's what they [rats] eat. And so with our campaign, we’re planning a lot of TV advertising, to teach people. The campaign is called Basket In. Basket in the trash. You have to start somewhere. There is so much commitment to look in every direction and make changes, all the things that really will make a difference to being sick and being healthy.
Over the years, SOMOS has used eHealth and digital services to allow secure exchanges between patient records which has helped establish better liaison between patient and doctors. Going forward, how does SOMOS intend to establish its digital outreach to meet growing demands?
Today, we use three or four platforms for review. We send protocols by electronic medical record, which we review by a corporation we call Optimus, where we were able to improve quality and review as we sat down with patients. We also established in February, when the pandemic was growing, telemedicine which we were able to share with patients. With telemedicine we were able to help so many people, not only our patients but anybody in a different language. We also established our practices within the district for mental health: PHQ-9 and GAP-7 screening, which were very important in knowing about sadness, anything that could help a patient with anxiety or depression and then we could refer them to specialists.
What are the challenges that you faced in bringing mental health care to communities of color, and why is connecting culturally sensitive healthcare providers integral for effective care (both mental and physical healthcare)?
Not only financial resources, but because [mental health] is personal, we have to employ more people that look like us, think like us and live in the community. Out of more than 200,000 patients, we find out that in the Bronx, 50% of the people in the Bronx speak Spanish, while only 10% of the healthcare providers do so. You have to do it [provide healthcare] in the cultural manner, it’s a necessity to the language, to the needs. In our case we do that and we know that we’re part of them. And I believe that as a person in charge of healthcare and its standards, we need to ensure that we get a new professional healthcare, which delivers services to the places that they come from, where there are people with need. We need to bring back the family doctor of the neighborhood, a gatekeeper who works together with the family, and sees the patient as a whole, not just a transaction before service.
